
When it comes to getting the most out of your doctors visits, I could tell you that the most important things to do are not to miss your appointments, take all your medications as directed, listen to your doctor and do every single thing he or she tells you. Those are all good things, but they’re things you’ve probably heard before. So I’m going to give you my own personal perspective, from a doctor’s point of view, on the top five things I think will be the most helpful for you. The good news is, it’s all very simple stuff.
Tip # 1: Be Honest
Do you ever feel like when you go to the doctor it’s like getting called to the principal’s office? You dread the appointment, you don’t want to know what your A1c is, you don’t want to hear the runaround again about what you should be eating and why you should take your medications. You also feel bad about how high your blood sugars are. People tend to get a lot of anxiety around this time.
It turns out that being honest with your doctor will not only not get you in trouble, it will help you get better. When you come to the doctor’s office and you’re honest, you should be rewarded for it, and you will probably get better medical care. If you don’t feel you can be honest with your doctor, then you might need to think about finding a new provider you can be honest with.
Let me give you an example of this. Here are two blood sugar logs from two different patients of mine on the same day in 2013:
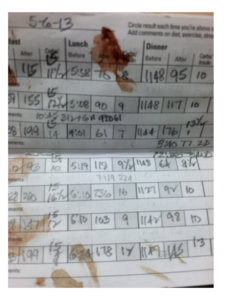
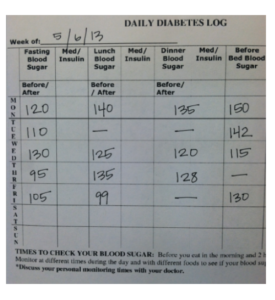
Which log do you think I like better?
The left one, because it’s a mess and I can tell it’s real! It has blood stains all over it and you can tell it’s really been used. This patient is being very honest. The log on the right is way too fishy. It’s super clean, no food has been near it, there aren’t any blood stains on it, and it’s fascinating to me that almost all of this patient’s blood sugars end in 0 or 5.
The patient on the right is not being honest. I consider this a failure on my part because I haven’t made her feel comfortable enough with me to be honest about her blood sugars. If someone comes in with this type of log and I believe it, that’s going to get both of us into trouble because I’m either not going to adjust her medications because things look too perfect, or I may cut back on medications and then all of a sudden she’s running out of refills too quickly because I’ve cut back on them since things looked so good. So it doesn’t help either one of us to fudge the numbers.
Another thing you can be honest about is food. This is one of the hardest things to be honest about, but if you’re not honest about what you’re eating, I can’t help you. You should not feel like you have to pretend not to eat carbs just because you have diabetes. And as it turns out…carbs are absolutely allowed if you have diabetes! Carbs are part of a healthy, balanced diet. If we (the doctors) know how you are eating carbs, we can help you adjust your diet to add carbs in the most healthy way.
One example is the type of carbs. One of the easiest interventions is if somebody tells me they’re drinking sugar – Red Bull, orange juice, regular soda, etc. If a patient changes to no-sugar, no-calorie drinks, we can sometimes get an A1c reduction better than most medications. Wow! I’ve seen A1c’s drop three points based on that change alone.
Another example is the amount of carbs. If you tell me you like to have four tortillas with rice, beans and cheese for dinner I may say, “Okay, can you do three tortillas?” Because that can have an impact. Your diabetes provider should work with you to find a way to try to make some modifications that will help your blood sugars.
My general guidelines for carbs are to tell patients to try to eat about 45-60g of carbs per meal. That may not sound like a lot, but if you have a turkey sandwich with bread from the supermarket, the slices are about 15 grams of carb each, so if you have two slices with some turkey and cheese, you’re only at half the carbs for that meal.
I gave this carb range to one of my patients and she came back to me later and said “Doc, I’m so proud of myself. I’ve been sticking to less than 60g of carbs per meal and I’ve been keeping a food log.” So I looked at her food log and this was my favorite entry: for breakfast one day she had a Slim Jim, 2 York Peppermint Patties, 2 Reese’s Peanut Butter Cups, 2 Andes mint candies and a Diet Pepsi. She counted all the carbs and it was only 49.5g. And do you know what I said? I said, “Way to go! You stayed within your carb limit!”
Now I’m not saying I promote that way of eating, but this was my patient being honest with me and working hard to follow instructions so I had to applaud her for that. It was a big carb reduction for her. Next we worked on incorporating more healthy carbs and less “junk food” carbs in her diet.
So be honest with your doctors! This is probably the most important thing you can do.
Tip # 2 Bring Your Medications to Your Visits
This is really important. I can’t tell you how many times we play the guessing game here. If I’m seeing a new patient or a patient in the hospital and I ask what they’re taking for their diabetes, some people will say, “It’s the little orange pill, and the round white one…” This may be a shocker, but doctors don’t know what your pills look like! They prescribe them, but they never actually see them. So it’s really important that you bring your pills with you, as well as your insulin. Insulins can get really confusing (especially insulin pens) so if you bring them in, we can help make sure you are taking the correct dose and type of medication.
Tip #3: Bring Your Diabetes “Stuff”
When I say stuff, I mean your good old-fashioned glucometer, your CGM if you’re on one, your insulin pump, your logs if you’re using logs…bring it all!

Diabetes is different than any other disease. With diabetes, we need to see your stuff because without that information, we can’t do anything.
One common reason patients do not bring their stuff is because they don’t want their provider to see the data. Maybe you’re not checking your blood sugars because you don’t want to see the numbers, but just because you don’t see them doesn’t mean they’re not high. So go ahead and check, and that way both of us can learn. For example, for most of my patients, I tell them to go ahead and eat their favorite food or splurge and then check their blood sugar. Go ahead! Give yourself permission to check after you eat half a pizza, or a huge bowl of ice cream, or a bag of chips! This is a great way to learn about how different food/carbs affect your body and then adjust your behavior to make your sugars better. Additionally if we don’t have the data, we can’t help you figure out why you are having highs or lows at a particular time of day. These are just a few reasons to bring all your stuff. With diabetes, information is key.
Tip # 4 Think About What Makes Your Diabetes Harder for You
This is really important. I don’t think a lot of people have actually sat down and thought about this. I’ve had so many visits with patients that are just us talking about everything besides blood sugars and diabetes medications. Can you think of all the millions of things that affect your diabetes? Stress, work, kids, partners, family, finances, menstrual cycles, acute sicknesses (cold, flu, etc) …all of those things affect your diabetes and it’s important for you to talk to us about them.
So what’s the hardest thing for you? Is it remembering to take your medication? Is it seeing high blood sugars? Is it sticking to a diet? Is it feeling like you’re always failing? Is it the cost? Don’t let people prescribe you medications you can’t afford. You’re not going to take them and then everybody’s going to be confused as to why your blood sugars haven’t gotten better, and it’s because you can’t pay $300/month for medication.
Or is the hardest thing just having a disease to deal with and think about every single minute of every single day? Sometimes talking about it can make it better, and sometimes your doctors or CDEs can find a way to help you through it. I can’t tell you how many times I’ve had conversations with people and I haven’t changed any of their medications, and things got better. Maybe we can find resources to help you deal with all of the other things in life you’re trying to juggle along with your diabetes.
Tip # 5: Ask How to Communicate Between Visits
I think sometimes people go to their doctors visits and then think, “Okay I’ve got that box checked and now I don’t need to do anything for my diabetes for the next three months until I go back for my next visit.”
But diabetes is not a disease that only doctors manage. It’s not something you take a pill for and then don’t have to think about. The whole purpose of TCOYD is to encourage you to take control between your doctor visits and make your own adjustments. Many people with type 1 do this all the time – they make adjustments with insulin pumps, insulin doses, etc., and people with type 2 should feel empowered to do that too – just get the education to do so with the help of your diabetes provider.
You should also discuss the following situations with your provider so you can be prepared if something comes up between appointments:
Know what to do if:
- You need a refill
- Your medications don’t get approved by your insurance
- You have a low blood sugar
- You have a high blood sugar and you just can’t get it down
- You need to have a phone call or visit with a nurse if you need something between visits
Remember, you are the co-pilot of your diabetes along with your provider. You decide together what medication is best to add next, how to manage your diabetes overall and how to do it between visits. Taking on that role is extremely important. The people who are actively participating in their diabetes between visits are the people who are most successful.
So these five tips may seem pretty simple, but I truly feel they are the most important things you can do to get the most out of your visits with your doctor.


New concept eat a healthy “diet” stay (or get) active. Use insulin to handle carbs (like the body does)..AND understand how it all works. New CGM technology like the Libre14. makes this do-able Yes food choices , activity , weight reduction may work for many T2D. The possibility of overlooked LADA(Latent autoimmune diabetes) exists subbest c-peptide test, pre-diabetic? ,how about an A1C. Just don’t take it lightly. It’s a progressive disease.
I have had Type 1 diabetes for 35 years. It is difficult to have to deal with this 24/7. But, generally, things have gone fairly well. TCOYD has helped me answer some questions. Thank you.
Thank you Carol, and congrats on 35 years – that is really something to be proud of. We’re glad to have helped with some of your questions and thank you for being part of the TCOYD family!
I agree that it would be best to be prepared if something came up between visits. I feel like it would be good to know what to do so that you won’t have yo wait until the next appointment to get help. Hopefully, that could help prevent some mistakes when it comes to medication refills and usage as well.
Yes, we agree!
I have had T1D for 38 years and it sucks! I am just reading the information on this website for the first time and am bummed out that I have not learned about TCOYD sooner and I missed the conference! Is there a way to sign up for e-mails?
Hi! Glad you found us! 🙂 We have a monthly digital newsletter you can sign up for on the home page of our website (towards the bottom) and if you would also like us to send you email notifications for conferences in your area, send me an email with your name, city and state and I can add you to our database. My email address is lynne@tcoyd.org. Our ONE Conference & Retreat for adults with type 1 will be in August again next year in San Diego – hope you can join us!
Soooooo I have had Type 1 for over 55 years!!! I don’t think there are many of us around…. I JUST found out about this website from a friend….soooo EXCITED to be able to attend your October conference in San Diego!!!
Thank you for doing this for us!!!!
Woohoo! Your excitement is contagious!! And congrats on 55 years – you rock! Happy you’ll be able to join us in October! 🙂
Yet another post I’m going share with my buddies on facebook. Thanks!
Thanks Tulia! 🙂
Excellent suggestions! Additionally, I recommend listening to lectures or podcasts that cover the most recent diabetes medication guidelines from the American Diabetes Association (ADA) and the American Association of Clinical Endocrinologists (AACE). This will deepen patients’ comprehension of how their physicians’ treatment strategies align with current care standards. I commend TCOYD for their efforts in this area. Your work in educating and enabling the public to actively participate in their health journey is truly commendable.
Thanks Vinny, and thanks for your additional comments!