
The musculoskeletal system (your joints, muscles, tendons, ligaments, bones and how they all work together) is quite commonly affected by diabetes. Some musculoskeletal conditions are unique to people with diabetes, but others are the same as those seen in people without diabetes; however, they may occur at a higher frequency among people with diabetes. Many of these conditions are treatable, but you must first recognize and identify them. In this article, we’re going to focus on conditions of the hand because diabetes can affect the hands in a number of ways, and our hands clearly play an integral role in our daily life.
Diabetic Cheiroarthropathy
Also known as limited joint mobility syndrome (LJMS) or diabetic stiff-hand syndrome, this condition is very much what it sounds like. Over time, the skin of the hands often becomes thickened, waxy, and tight, especially on the back of the hands and fingers. This results in limitation of joint movement, especially the small joints of the fingers, producing a decreased ability to bend and/or straighten them. The fourth and fifth fingers are typically affected first. It is generally a painless condition but can have a big impact on the ability to use hands normally. The “prayer sign” observed in this condition is an inability to flatten the palms together completely, with a visible gap remaining between the opposed palms and fingers.

Stiff Hand Syndrome occurs in both type 1 and type 2 diabetes, and the risk is higher with increasing A1c values as well as with increased duration of diabetes. Nearly half of adults with type 2 have some evidence of LJMS. LJMS is difficult to treat and generally irreversible. Optimizing control of blood glucose is advised. Physical and occupational therapy with regular, gentle stretching of the fingers and palms may be helpful. When LJMS affects the feet, it may also be associated with an increased risk of foot ulcers.
Flexor Tenosynovitis or Trigger Finger
In our hands, fingers bend when tendons shorten (contract) and straighten out when tendons lengthen (extend). When there is an abnormality in the tendon or the surrounding tissue, the finger may actually become stuck in a flexed or bent position, requiring the use of the other hand to straighten it out.
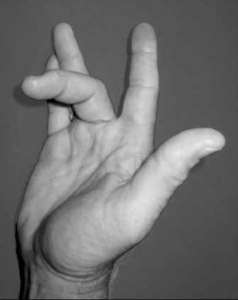
Flexor tenosynovitis (FTS) is caused by a thickening and fibrosis of the tendon or the tendon sheath that limits movement of the flexor tendon of the affected finger(s). FTS, or trigger finger, is a frequent musculoskeletal complication of diabetes and occurs more commonly than in the general population. Affected people complain of a catching sensation, or locking, of the finger(s). It is often painful, and there may be a nodule that can be felt on the palm at the base of the affected finger. Trigger finger is more common in long-standing diabetes and the risk of developing flexor tenosynovitis goes up as A1c levels increase. A local steroid injection may be adequate treatment, at least temporarily, but sometimes minor outpatient surgery is required for trigger finger. Treatment with local steroid injection may be less effective in patients with diabetes compared with those without diabetes.
Dupuytren’s Contracture
Dupuytren’s contracture results from a persistent thickening and shortening (fibrosis) of the tissue (fascia) just under the skin of the palm. The result is permanent bending (flexion) of the finger(s), particularly the third and fourth fingers in people with diabetes. The area often feels thickened and has bands, bumps, or nodules along the palm. Dupuytren’s contractures tend to interfere with “gripping” activities but are not usually associated with pain. The frequency of Dupuytren’s contracture is higher in people with diabetes and increases with the duration of diabetes, and is also associated with the presence of peripheral neuropathy in type 2 diabetes.
Dupuytren’s has a variable course. For mild cases, gentle stretching of the fingers and palms a few times a day is recommended (you can use a tabletop to try and get the hand flat along the table surface). For more advanced cases in which function is affected, steroid injections may be tried, but are not very effective in long-standing cases. Surgery may be done for extreme cases, but the recurrence rate is high. More recently, injection of collagenase has been tried with some significant improvement seen and is an (expensive) alternative to surgery.
Carpal Tunnel Syndrome
Carpal tunnel syndrome (CTS) is due to compression of the median nerve as it passes through the palm side of the wrist into the hand. In people with diabetes, this compression may be due to thickening in the connective tissue of the wrist caused by high blood glucose. Affected people often notice a burning pain, pins-and-needles sensation, or loss of sensation in the hand, most commonly in the thumb, index, and middle fingers as well as half of the ring finger. Pain may radiate up the forearm. Symptoms may be worse at night and can be worse with activities such as driving, holding a newspaper or book, typing, or using a knife and fork. There may be associated loss of dexterity or weakness of the hand.
CTS is seen in up to 20% of people with diabetes, and people with diabetes are at three times higher risk of developing CTS than people without diabetes. The finding of CTS is related to the duration of diabetes. If CTS is not severe, initial treatment consists of using wrist splints. Anti-inflammatory medications may also be tried (such as ibuprofen). Local steroid injection of the carpal tunnel is another option. For severe or refractory cases, carpal tunnel release surgery may be performed.
Summary
These conditions can have a significant impact on the quality of daily life of people with diabetes, but many of the complications are treatable, offering improvements in quality of life and daily activities. It’s important to be aware of the possible ways in which diabetes can affect your musculoskeletal system, and discuss any concerning symptoms with your doctor or rheumatologist.

Thank you for this article. I have had problems with my hands and wrists for almost 30 years and have had T1D for 56 years. I have had carpal tunnel and trigger finger surgeries on both hands, as well as enzyme injections for Dupuytren’s contracture. My hand surgeon has been telling me that this is one of the complications of long-term diabetes. My sister, who has had T1D for 49 years, has been “following in my footsteps“ with her hand and wrist surgeries. I appreciate the descriptions in the article.
Yes, they are all very common, but you are in an elite group with me now!
Thank you Dr. Edelman for this information. I have had Dupuytren’s contracture in both hands for 25 or 30 years. I have had diabetes, type 1, for 45 years. I recently saw a hand surgeon for a trigger finger. He told me the trigger finger was from diabetes but the Dupuytren’s was not from diabetes. I had always thought the diabetes had something to do with this. I declined the steroid injection for the trigger finger and am holding off on surgery for now. The surgeon told me doing surgery on the trigger finger could cause more problems with the Dupuytren’s. Any recommendations for nighttime pain excluding NSAIDS? FYI, I am a nurse and CDE, recently retired, and have always had excellent control. Thanks.
I have had four trigger fingers…three of them I went to a very good hand surgeon at UCSD where they inject steroids first, but it did not help, so I had surgery. All three are excellent now without any issues or worsening Dupuytren’s. My fourth did respond to local injection of steroids and I’ve never had another problem with it. Both Dupuytren’s and trigger finger commonly occur in people with diabetes. If I were you I would definitely try injections first and if that doesn’t work have surgery, but find a good hand surgeon. Based on what you’ve told me I’ve lost confidence in your doctor, but obviously I don’t know him. Regarding your other question, Tylenol is much safer for people with diabetes. You can also try tramadol but that requires a prescription.
Thank you so much. I appreciate your time and information. I will check out hand specialists in Kansas City.
Yes I had about 4 or 5 trigger fingers done surgically and they are all great now, they tried injection and first the injections are very painful and they don’t work after the second one my doctor said, we have to do surgery and that worked great. I had that done about 3 years ago and never had another one. I suggest don’t go to the injection, do the surgery it’s easy and it works.
Surgery does work well on this issue, and your experience is a common one! Thanks for your comment!
Hi Dr E! Why does this article not talk about the use of radiation treatment for Duputren’s contracture? I had it done years ago at Scripps with Dr Tripuraneni and it stopped it in its tracks. I know it will never go away, but if it stops it from progressing, then I think it’s worth talking about and letting others know there is another treatment to explore. Just thought I’d share!!
Hi Karen,
Thank you for the comment. The rheumatologist who assisted in writing this article is at the University of Toronto, and I’m guessing they do not use radiation therapy. I didn’t know that myself, and I had Dupuytren’s contracture, but luckily not that severe. Thanks for the heads up and we’ll let her know.
Thank you for the article about trigger finger!
I want to share that I had trigger finger; and my trigger finger is gone by reducing my A1C without injection.
I was diagnosed 10 years ago with type 2 diabetes and my A1C was 9.3. I was determined to reduce my A1C with exercise and diet without medication. I was able to reduce my A1C down to 6.3 in 2 years then I had a baby and A1C went up again to 8.3. I started to experience stiff hands in the morning and trigger finger about 3 years ago. My arthritis doctor suggested injection for trigger finger. My first TCOYD conference at Santa Clara 2019; and I learn about the Stanford Asian Diabetic Study(normal weight) and became a participant. I had to follow exercise guide line during the study. I was able to reduce A1C down to 6.5 in 9 months and the trigger finger and burning foot symptoms(started during the beginning of the study) are gone. EXERCISE and DIET are great medicines for me. P.S. I did have burnout moments. It is hard! Just keep going!
Good for you, and great motivation! 🙂
I have trigger finger on my right hand. Three weeks ago I had a steroid shot. I assumed the diabetes was the reason for the trigger finger but the doctor never mentioned it. He just said it was either a shot or surgery. The shot hurt like crap! My finger is better but not completely healed. I have been reading articles that given time, trigger finger will heal itself. Not true? Just wondering about the healing. Thanks for the information above.
In my clinical and personal experience, the steroid shots do not make a big impact, and the surgery is typically really easy and quick but make sure you go to a hand surgeon that has experience.
Reading up possible treatments for my dad’s trigger-finger condition. This article has been insightful.
Sadly, he passed away September 11, aged 82. We did our best. He lived a good life.
I am a diabetic and I have had carpal tunnel surgery, and trigger finger surgery on both my thumbs. I am now waking up in the mornings with trigger finger on finger next to my little finger on my right hand. I had rather have the surgery than have the painful injections. I’ve started taking vitamin E and C at night, hoping it will help.
Hi Linda,
To be honest, I don’t think the vitamins will help and I also totally agree with you – it’s much better to have the trigger finger surgery than the injections, which rarely lead to permanent success.
Please see below…
At least for me regarding the shots for Dubuytrens, my affected fingers were treated with several shots on both hands over the course of a couple of years The ortho doctor said after three shots that didn’t work, surgery was needed. For the one finger that was still affected, I talked him into giving me a fourth shot. That worked. I’m thinking it may just take an extra shot for a T1D whose been diabetic for 50+ years?
I have had T1 diabetes for 40 years. I was diagnosed with Dupuytren’s contracture, most severe in my dominant left hand. I am thinking now that I may have diabetic hand. I have constant pain and stiffness in my hand. I cannot grip anything. I had never heard of diabetic hand until today. Would radiation therapy work for diabetic hand? I am a medical transcriptionist and typing is becoming more and more difficult. I don’t know what to do for pain anymore.
In my experience, going to an excellent hand surgeon can make a huge difference.
I’m 52 in great health with no health problems. Ive lost the ability to bend my first and ring finger on my left had in just over a month. It’s very painful and if I press on my joint on the palm side.. That’s where the pain is. Could carpal tunnel cause that?
Most likely not. I would definitely see a hand specialist.
I have had progressive symptoms consistent with LJMS for a few years, but over the last few months it has.become painful in both hands, worse on right. Is there any known treatment in addition to trying to improve glucose. Quality of life is now being diminished greatly.
Absolutely. Sometimes injections of steroids are used, but it sounds to me like you need a very good hand surgeon. The surgery is simple, quick, outpatient procedure, and could change your life.
I’m considered pre-diabetic with an A1C of 6.3, but I had sudden onset of multiple trigger fingers, stiff hands, painful joints and loss of function about 1.5 yrs ago. Trigger thumb resolved in the months it took to get in to see a hand specialist, but other 2 (long fingers on both sides) did not respond to steroid injections or oral NSAIDS. I’ve been putting off the recommended surgeries due to life at the moment.
Is it possible that pre-diabetes could result in this condition? I’ve seen 2 different rheumatologists and all labs for the usual autoimmune joint diseases come back negative. I do have Hashimoto’s that has been poorly controlled in the past.I’m finally scheduled to see an endocrinologist, but the soonest I can get in is November. Thank you
It is possible, however your case seems a little bit more aggressive than the ones I’ve seen. I would not delay surgery because it’s super easy, there’s no need for general anesthesia, and it’ll help relieve your problems. I personally have had three trigger finger repairs myself, and my only regret is waiting too long. The injections did not work at all for me.
The other thing I want to mention is if you have painful joints and loss of function, there may be another diagnosis that’s being missed if we’re only assuming it’s isolated trigger finger. I would recommend finding a good rheumatologist to work you up for maybe a different autoimmune problem because of the aggressive nature of what you’re describing.
About ten years ago I had terrible pain in my fingers especially in both thumbs. My thumbs actually became deformed. I discovered the pain was caused by artificial sweeteners creating inflammation in my joints. I immediately stopped all artificial sweeteners and the pain went away although my thumbs were still deformed and weak. I had to work on building strength back in my hands and now they work pretty well with no pain. No one seems to believes that the sweeteners could do this damage but I definitely had a reaction to them. I’m a 73 year old with LADA type 1.
Artificial sweeteners typically do not cause that and I haven’t heard of it before, however, in medicine you never say never and you never say always. You may have had a bad reaction to the one that you were trying. It sounds like you are better, at least to some degree. Good luck, and hope you have continued progress.
Thank you. Type 1, adult onset, for about 40 years. I have or have had all of these! Couple of Duyputrens surgeries later I thankfully can use my hands without pain. More to come, no doubt.
Thankfully the surgeries are pretty straightforward and can get people back to normal function fairly quickly.
You did a great job illustrating Stiff Hand Syndrome in a recent podcast. After having pretty well controlled T1d for 43+ years, I never experienced any musculoskeletal hand problems UNTIL…
I fell and broke my wrist, it heeled poorly (mal-union) and I had surgery involving installing a metal plate and screws.
After a few weeks of post-surgery occupational therapy, I cannot hold that hand flat against a surface or against my other hand (prayer position) I also cannot make a tight fist or actively touch my thumb to my pinky. My hand and 3 fingers feel numb and “tight” and “pin cushiony”. The palm on that hand is dry and scaly (maybe unrelated). The surgeon was very good but maybe not knowledgeable about the diabetes connection. Could the combination of long term T1d (again, well-controlled a1c=<6.5 but for a looong time!) plus the surgery have combined to cause this?
Note, If I passively straighten fingers it helps for a while and they are then painful when I try to make a fist. It's like I imagine arthritis would feel like.
Should I push to get another surgery or shots?
Wow…amazing journey with the hand. I do think that something happened when you fell and broke your hand. If it was classic MS issue it would have started and slowly gotten worse. It is hard to tell from afar. I would see a different orthopedic hand specialist. Hang in there!
My rheumatologist said I had diabetic stiff hand syndrome but my a1c is 6.3 but I have had t2 diabetes for50 years so is it caused by long term insulin use and what can you do because my blood sugars are quite low. Is there any medication or therapy?
Having diabetes for 50 years is your biggest risk factor and at this point, glucose control is not an issue. Do stretching and strength exercises (get a puddy ball and squeeze the hell out of it!). If things do not improve, perhaps a PT or OT person.