
What Are Screenings?
Health screenings begin before we take our first breath. Pregnant mothers undergo prenatal screenings to determine their and their baby’s health risks. More often, screenings are performed to identify conditions in which interventions can lead to better outcomes. When babies are born, they undergo more screening, known as newborn screens.
These screenings accomplish two tasks: detecting current life-altering conditions, such as sickle cell disease, and identifying risks for diseases, such as cystic fibrosis. Screenings do not diagnose conditions, but lead to further testing to rule in/out a disease or health condition. Screenings are the foundation for primary care, the reason we go for annual visits and take our children for well-child checks. Whether for hearing proficiency, visual acuity, anemia, or autism, children have screenings at every age. Multiple screenings continue through adolescence and adulthood, targeting various treatable health conditions such as elevated cholesterol, cancers, cardiovascular risks, and diabetes. Screening for diabetes is commonplace, but mostly for type 2. This is because screening for type 1 diabetes (T1D) used to be limited to research settings. However, screening for T1D has become more practical to do outside of research. In fact, it can be done by your healthcare provider, at a lab, or in your own home.
Why Get Screened for Type 1 Diabetes?
No one wants a positive screen for themselves or a loved one. It can be frightening and overwhelming. However, ask yourself, what’s worse? Knowing or not knowing? You might be wondering how knowing that you or someone you care about has early stage T1D will change anything. Understanding more about the risk, development, and progression of T1D may help answer many questions you or your loved one may have. A good place to start is by having a conversation with your (or your child’s) healthcare provider.
From a parent’s perspective, these difficult thoughts and questions can be a key contributing factor when either seeking to understand and accept a potentially life changing event or choosing the “ignorance is bliss” approach, letting the potential event happen as it may. This is not a right or wrong proposition and should not be taken lightly or acted upon impulsively. This decision, although ultimately pertaining to a single loved one, has the power to affect all members of the family. Alignment, communication, and, most importantly, support are key factors to overcoming any obstacle or challenge as a family. This decision should be viewed no differently. Sitting down and discussing the “what ifs” and the “pros and cons” can potentially lead to questions, which often lead to knowledge, which ultimately leads to power over your potential fears. Creating a list of the pertinent points related to what can happen if we do vs. what can happen if we don’t, can be a useful tool in helping families make this critical decision, ultimately bringing loved ones together in the process. Your child may have questions, thoughts, or fears that should also be addressed at this time. Love is, and will always be, the answer, and whatever decision is made, know that you and your child will not only get through this, but overcome this together.
What Are the Stages of T1D?
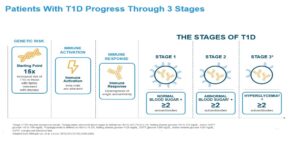
T1D has three progressive stages of disease, and its course is highly predictable. In all three stages, a person has a positive blood test for T1D autoantibodies. Autoantibodies are a signal that the body’s own immune system is attacking the pancreas. Stages 1 and 2 are early and often pre-symptomatic, meaning people do not have symptoms of this immune attack in their body. In stage 1, a person still has normal blood sugar control. In stage 2, a person is starting to have abnormal blood sugars, but they do not yet need to take insulin. In stage 3, a person’s blood sugars are higher than normal because their bodies no longer make enough insulin.
Who’s At Risk?
Approximately 1.6 million Americans have T1D, and the number of people being diagnosed is steadily increasing by about 2% each year. Individuals with a family history of T1D are at higher risk of disease. However, surprisingly, 80-90% of people newly diagnosed with T1D have no family history. It is estimated that 300,000 people in the U.S. today are at risk for developing insulin dependent T1D. Because stage 1 and 2 are early in the disease spectrum, people often don’t know that they have it unless they are screened/tested. If someone screens positive for two or more TID-related autoantibodies, then further evaluation is needed to determine the stage of T1D. If someone is in stage 1 or 2, then the risk of progressing to clinical stage 3 T1D is nearly 100%. It’s not a matter of if someone will need insulin, but really, it’s a matter of when.
What’s Happening Today?
Most people are currently diagnosed in stage 3 disease once they become symptomatic. Typically, the symptoms include excessive thirst and urination, fatigue, and unintended weight loss etc. When diagnosed in stage 3, a person must begin to take insulin to survive. Approximately, 60% of people diagnosed with T1D in the United States today present in diabetic ketoacidosis (DKA). DKA is a life-threatening medical emergency that requires hospitalization. In severe presentations, it may lead to brain swelling and death. Additionally, people who experience DKA can proceed to have long-term difficulties with blood sugar control and may develop cognitive deficits. Currently, screening for T1D autoantibodies in the United States can be done in three ways. One, a healthcare provider can order a blood test. Two, a screening can be performed through participation in a research study. Three, individuals can order an at-home blood test (through JDRF’s T1Detect or TrialNet).
What Next?
Healthcare professionals are readily available to support individuals and walk patients through screening and diagnosis. People should seek guidance from their healthcare provider regarding their screening results. Healthcare providers can advise on frequency of re-screening for those who screen negative or those who are positive for one autoantibody. For those who screen positive for two or more autoantibodies, further evaluation may be needed to determine blood sugar levels and stage of disease. Primary care providers, endocrinologists, and diabetes specialists can order additional tests to make these determinations.
People with early stage (stage 1 and 2 T1D) have an opportunity to learn how to manage their blood sugar levels before they get dangerously high. This can potentially prevent DKA and hospitalization. In addition, the T1D community is tight-knit and robust with many support groups. Advocacy groups, such as JDRF and TCOYD, have a plethora of information and resources available to families affected by T1D.
Health screenings provide us with information about what is occurring in our bodies. There’s an old saying that knowledge is power. Understanding a disease can restore the power that the diagnosis takes away. It provides an opportunity to seek out information and make decisions regarding treatment before it progresses to an advanced stage.
Resources used for this article and additional information can be found at:
https://diabetesjournals.org/care/issue/45/Supplement_1 American Diabetes Association Standards of Medical Care in Diabetes—2022. The Journal of Clinical and Applied Research and Education-Diabetes Care, volume 45, supplement 1
https://www.jdrf.org/t1d-resources/hcp/#screening Next Steps for Patients and Families After Screening for T1D Autoantibodies

Great content! This is exactly the sort of thing I was looking for. Thanks for your help
An excellent perspective! Thank you.