
Medically reviewed by Dr. Steve Edelman
Everyone has their fair share of obstacles to overcome with diabetes. I have had type 1 diabetes for almost 20 years and have experienced many challenges; however, there is one that doesn’t seem to get as much attention as others: lipohypertrophy. If you don’t know what this is, or if you’ve experienced it but don’t know how to solve it, we’re going to delve into this often overlooked problem and offer a few solutions.
What is Lipohypertrophy?
Lipohypertrophy, commonly referred to as “insulin bumps,” is a medical condition often seen in individuals who regularly administer insulin injections. It manifests as localized, raised areas that can feel like a bubble under the skin after an insulin injection. These bumps arise due to repeated injections in the same spot, leading to a buildup of fat tissue.
What Dose Lipohypertrophy Look Like?
Lipohypertrophy is characterized by the formation of firm and dense bumps around injection sites on the body. The lumps are buildups of fatty tissue that develop under the skin when an insulin injection site is used repeatedly or too often. Though the size and shape of these bumps can vary, this condition can happen to anyone who takes insulin through injections or infusion tubing from pumps.
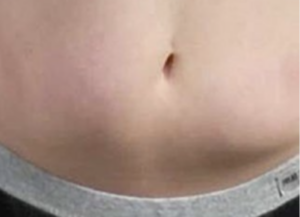
My Experience with Lipohypertrophy
In my 20+ years of living with diabetes, I’ve administered insulin both through infusion sets from an insulin pump and with a syringe when I was on multiple daily injections (MDI). My abdomen is a spot that I like to use for both injections and infusion set insertions. While avoiding the belly button, I pick a spot where I’ve had more consistent glucose levels. Although I tried rotating injection sites as often as possible, over time I noticed that after using that common spot repeatedly, it felt lumpy, firm, and somewhat raised. Usually, the area is about the size of a quarter or half dollar. If you’ve noticed something similar happening in an area where you inject a lot…that’s lipohypertrophy.
Why Do I Get a Lump After Injecting Insulin?
The main reason is due to the action of insulin on fat cells, because insulin can cause them to increase in size. This process is known as lipogenesis. Approximately 64% of people with diabetes will develop lipohypertrophy at some point in their life. Personally, I started noticing it about 15 years after my diagnosis. At that point, I had been on an insulin pump for about 12 years. The first thing I noticed was that my infusion set was leaking insulin after giving a bolus. Then came spikes in my blood sugar. It was only after I removed my infusion set that I noticed the signs of lipohypertrophy.
What Causes Lipohypertrophy?
The primary cause of lipohypertrophy is failing to rotate or change injection or infusion sites regularly, but even if one rotates or changes injection sites frequently, it is still possible that lipohypertrophy could develop due to the lipogenic action of insulin. Then why rotate insulin injection sites? Research has shown that correct rotation techniques have the highest protective value against the formation of lipohypertrophy.
How Does Lipohypertrophy Affect Insulin Absorption?
Lumps from lipohypertrophy become problematic when insulin injected either around or into these sites is not well absorbed. Therefore, the insulin will not lower your blood glucose as efficiently. One reaction to this might be increasing your insulin dose to compensate. However, if you inject a higher dose in a spot not affected by lipohypertrophy, you run the risk of hypoglycemia.
The American Diabetes Association conducted a study in 2016 that tested the effects of insulin absorption in people with type 1 diabetes who received insulin via injections. Compared to a control group of people with normal tissue, those with lipohypertrophy had low insulin absorption. In addition, postprandial (after meal) blood glucose levels were about 26% higher for those with lipohypertrophy.
Even with the highs and lows that can come with lipohypertrophy, it’s possible A1c levels won’t be affected. However, a variance in blood sugar could affect time in range.
Lipohypertrophy Treatment and Prevention
One of the strategies I personally use to avoid lipohypertrophy is to frequently check my sites in front of a mirror. The abdomen is one of the most common spots I use for my infusion sets and injections. I’ll usually stand in front of a mirror and check around sites for any bumps, or for any dips that could be around bumps. By comparing the right and left sides I can see differences, and then I feel around each side for any developed bumps. Usually, a spot that is hard and dense indicates a spot where lipohypertrophy has developed, which means I will stay away from injecting near that spot for a while. When choosing new injection sites, I will try to stay away from any bumps by a distance of about two fingers (minimum).
Unfortunately, there aren’t any medications to prevent or cure lipohypertrophy. The best thing to do is to try to avoid using sites where lipohypertrophy has occurred. There is no definite timeline as to when these sites will completely heal. It can take weeks to months, and sometimes years. Recovery depends on how long lipohypertrophy has been present.
Strategies to Prevent Lipohypertrophy
Here are a few strategies you can use to try to prevent lipohypertrophy:
- Establish a plan that includes a schedule of sites and rotations.
- Rotate insulin injection sites. Here is a list of common sites used for insulin injections:
- Abdomen (about two inches from the belly button)
- Front of the thighs
- Back of the upper arms
- Upper buttocks
- Inspect your skin before injecting medication or inserting an infusion set.
Every time you have an in-person appointment with your diabetes doctor, consider having your provider inspect your injection and infusion sites, especially if there are areas that are red, bruised, painful, or warm to the touch. Also, let your provider know if you’re having trouble controlling your blood glucose levels.
How to Get Rid of Insulin Bumps
Unfortunately, there aren’t any medications to prevent or cure lipohypertrophy,. Tthe best thing to do is to try to avoid using sites where lipohypertrophy has occurred. Surgery and liposuction to remove fat deposits are resorts to treat severe lipohypertrophy.
Does Lipohypertrophy Go Away?
There is no definite timeline as to when these sites will completely heal. It can take weeks to months, and sometimes years. Recovery depends on how long lipohypertrophy has been present.
In Summary
Overall, lipohypertrophy is a common condition that can affect how people manage and control their diabetes. By understanding what it is and how to prevent it, you can maintain better glycemic control and prevent fluctuations in blood glucose levels. The importance of self-checking and having your provider check for lipohypertrophy lumps at in-person appointments cannot be understated. Creating an efficient schedule of injection and infusion site rotations can do wonders to prevent lipohypertrophy. Through these strategies, it is possible to prevent lipohypertrophy. In some cases where people have already developed lipohypertrophy, using these strategies can help allow the skin proper time to heal and help you get back on track with your insulin regimen, blood glucose control, and overall diabetes management.
About Aaron Albanez
I was born and raised in San Diego, CA and have been a type 1 diabetic since 2003. I have previously attended the in-person conference for TCOYD and have had the opportunity to volunteer with them. TCOYD is an organization I hold in high regard and have made strides in my diabetes management thanks to this wonderful organization. Diabetes is an aspect of my life that I have aligned with my career goals. I originally obtained my BS in Chemistry from UC San Diego, but have now shifted my focus on public health. I am currently working to obtain my Masters Degree in Public Health with an emphasis on Health Education and Promotion from the University of Alabama. I have worked in the healthcare field since 2017 and hope to be involved with diabetes management and care once I obtain my MPH. Outside of the office, you can usually find me roaming around Main Street in Disneyland with my wife, Oksanna.
Additional Resources:
Size Matters! All About Needles and Multiple Daily Injections

I sure wish this was something that my endo would discuss with me as well as inspecting my injection sites instead of just occasionally looking at my feet.
Definitely bring it up at your next appointment!