
- Even though some people may choose to ditch gluten because they think it’s trendy, celiac disease is a serious autoimmune condition that can often occur in people with type 1 diabetes.
- In celiac disease, the immune system mistakenly attacks the lining of the small intestine, so nutrients from food aren’t absorbed the way they should be
- Symptoms of celiac disease can be subtle or nonexistent in people with diabetes, which is why screening is so important.
- If left untreated, celiac disease can lead to long-term complications like osteoporosis, heart disease, and other autoimmune conditions.
- Treating celiac disease involves following a gluten-free diet, but you can still live a full, healthy life with both celiac and T1D.
Reading Time: 4 minutes
When you see an influencer swear up and down that cutting gluten from their diet makes them feel cleaner, less bloated, and full of energy, it’s only natural to give your whole wheat sandwich a little side eye.
Gluten-free living is often touted as a trendy fix for bloating or brain fog, but celiac disease isn’t a wellness fad – it’s an autoimmune condition that can show up alongside type 1 diabetes. In fact, about 6% of people with T1D have celiac, compared to roughly 1% of the general population.
So how do you know if gluten is just the buzzword de jour, or if it’s truly affecting your health? Keep reading to learn more about celiac disease and diabetes.
What Is Celiac Disease?
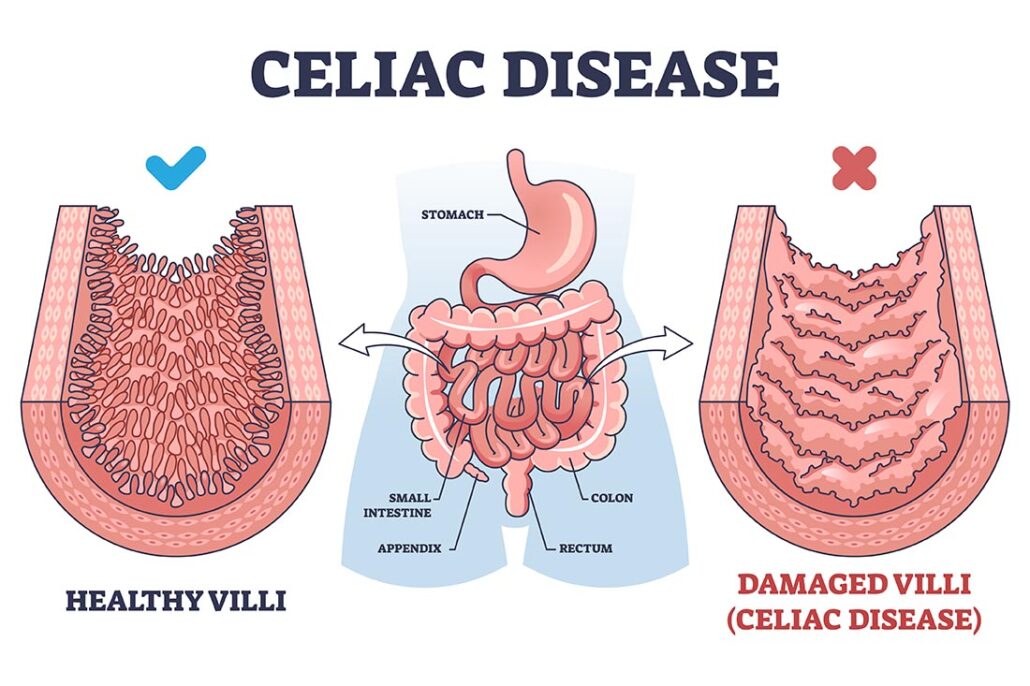
Celiac disease is an autoimmune condition that’s triggered by gluten, which is a protein found in wheat, barley, and rye. When someone with celiac disease eats gluten, their immune system attacks and destroys the lining of their small intestine.
Why does this happen? We really don’t know, but it’s similar to the immune reaction in type 1 diabetes when the body destroys the insulin-producing beta cells in the pancreas.
In celiac disease, the immune attack damages the tiny, finger-like projections in the small intestine called villi (not to be confused with Milli Vanilli), which are responsible for absorbing nutrients from food. When they’re damaged, nutrients don’t get absorbed the way they should. If left untreated, celiac can lead to long-term problems like osteoporosis, heart disease, and other autoimmune conditions.
If you have a first-degree family member with celiac (a parent, child, or sibling), you have ten times the risk of developing celiac as well.
Type 1 Diabetes and Celiac Disease: Why the Higher Risk?

When it comes to type 1 diabetes and celiac disease, certain genes that raise the risk for type 1 diabetes also raise the risk for celiac. Both conditions are linked to the human leukocyte antigen (HLA) genotype, but we’ll spare you the genetic deep dive…just take our word for it!
When you have T1D, your immune system already misfired once when it attacked the beta cells in your pancreas. When the immune system is in attack mode, it’s easier for it to “go rogue” again. Autoimmune diseases often travel together, so having one condition can increase the risk of developing another.
Even though many people with type 1 diabetes never get another autoimmune condition, it’s important to be aware of the connection so you can keep an eye out for new or changing symptoms and stay on top of recommended screenings.
Symptoms of Celiac Disease in People with Diabetes
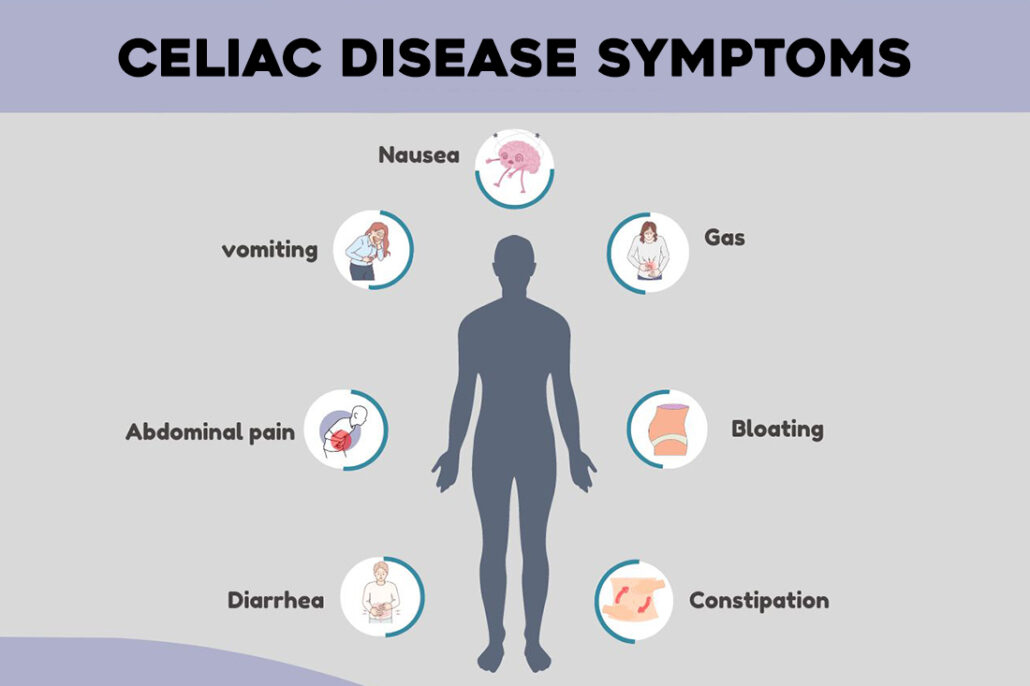
Signs of celiac disease aren’t always obvious, especially in people with type 1 diabetes. Some people experience typical digestive symptoms, such as bloating, abdominal pain, diarrhea, or weight loss. Others have very mild symptoms, or none at all.
Common digestive symptoms include:
- Abdominal pain
- Bloating and gas
- Constipation
- Diarrhea
- Nausea and vomiting
- Weight loss
Common non-GI symptoms include:
- Brain fog
- Anxiety and depression
- Delayed growth or puberty in children
- Fatigue
- Headaches
- Joint pain
- Iron-deficiency anemia
Since celiac disease damages the lining of the small intestine, it can interfere with how nutrients and carbs are absorbed, which can make blood sugar unpredictable. So if your blood sugars have been out of whack for a while for no apparent reason and you have some of these symptoms, you might want to talk to your doctor about being tested for celiac.
How Is Celiac Disease Diagnosed in People with Diabetes?
Because symptoms of celiac disease are often subtle or nonexistent in people with diabetes, screening is recommended at the time of T1D diagnosis, again within 2–5 years, or anytime symptoms appear.
Screening usually begins with a simple blood test that checks for specific antibodies your body makes in response to gluten. If those results suggest celiac disease, your doctor will typically recommend an upper endoscopy to confirm the diagnosis by taking a small sample of tissue from the small intestine.
How Do You Treat Celiac Disease and Diabetes?

We’re going to start with the good news…there are more gluten-free products and resources available today than ever before in the history of humankind. The not-as-good news is that the only treatment for celiac disease currently is to follow a full gluten-free diet. This means avoiding foods that contain wheat, barley, and rye.
If you’re already dealing with type 1 diabetes, this can obviously be overwhelming. But you don’t have to figure it out alone (and there is gluten-free beer to take the edge off!).
A dietitian who understands both type 1 diabetes and celiac disease can help you figure out a nutrition plan, and a counselor or therapist who specializes in chronic conditions can help you navigate the emotional side. You can definitely live a long and fulfilling life with both conditions.
Tips to Manage Type 1 Diabetes and Celiac Disease:
- Give yourself time to adjust, and don’t worry about being perfect from day one.
- Put your focus on what you can eat instead of what you can’t.
- Seek out a support group of people living with both conditions.
- Involve your friends and family, and tell them how they can best support you.
- Read ingredient labels…gluten can hide in weird places, like soy sauce!
- Take advantage of the diagnosis when you can! Get a note from your doctor so you can bring your own food into places that charge an arm and a leg for it…like amusement parks and sporting events!
Celiac Disease and Diabetes Frequently Asked Questions
🥖 How Common Is Celiac and Type 2 Diabetes?
People with type 2 diabetes can develop celiac disease just like anyone else, but there’s no established link between the two conditions. Type 2 diabetes is not an autoimmune condition, and it does not increase your risk for celiac disease.
🥐 How Is Celiac Disease Different from Gluten Sensitivity and Gluten Intolerance?
Celiac disease is an autoimmune condition that causes damage to the lining of the small intestine when someone eats gluten. With non-celiac gluten sensitivity, people may feel bloated, tired, or have stomach pain after eating gluten, but there’s no autoimmune damage. Gluten intolerance is often used casually to describe either celiac disease or gluten sensitivity, but it is not a formal medical diagnosis.
🩸 How Does a Gluten-Free Diet Affect Blood Sugar?
Many packaged gluten-free products are lower in protein and fiber, higher in saturated fat, and higher on the glycemic index. Some gluten-free products use added starches to improve taste and texture, which can raise their carb count. Insulin needs may change after a diagnosis of celiac, so keep your healthcare team in the loop about how you’re managing your new diet and its effect on your blood sugar.
Key Takeaways: Type 1 Diabetes and Celiac Disease
Even though type 1 diabetes does increase the risk of celiac disease, most people will never develop it, so you don’t have to chuck your ciabatta bread out the window just because an influencer says you should.
Since celiac disease can be asymptomatic in people with T1D, screening really matters. If you haven’t been tested, talk to your provider. If you test positive, removing gluten from your diet will make a big difference in how you feel, and you can still live a full, healthy life with both conditions.
If gluten isn’t a concern, keep on doing what you’re doing to manage T1D. Diabetes is already a full-time job and you’ve got enough on your plate, so go fill it with something you love, like a California burrito!
Explore our resource library and video vault, and subscribe to our monthly digital newsletter for more tips, tools, and expert guidance on how to take control of your diabetes.


Our goal is to protect your personal health information. Please keep your questions general and do not post personal medical information here. If you have a specific question, please email events@tcoyd.org.