
The Patient:
John is a 55-year-old man with a long history of type 1 diabetes. He currently uses the Tandem Control IQ hybrid closed-loop system, along with a Dexcom CGM. His 90-day Dexcom CGM download from his last appointment with me is below:
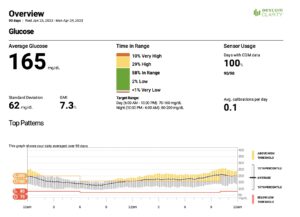
Here’s a breakdown of the data at a glance:
- His average glucose was 165 mg/dL. The target for most people is less than 155 mg/dL.
- His estimated A1c (GMI in the download) was 7.3%. The target for most people is less than 7%.
- His standard deviation was 62 mg/dL. Standard deviation measures the variability in glucose levels, and the typical goal to shoot for is less than 50 mg/dL.
- His time in range was 58%. Time in range (TIR) is defined as the time someone is between the target range of 70 and 180 mg/dL, and the goal is over 70%.
- His time below range was 2%. The goal is 4% or less.
- His time above range was almost 40%.
The Problem:
The number most concerning to me was his reduced time in range (TIR). When you look at his 24-hour glucose profile (the graph at the bottom) you can see that his blood sugars come down nicely overnight (midnight is on the left side of the graph). Once he has his first meal of the day though (in the late morning), his average blood sugar goes above 200 mg/dL and stays there for the rest of the day and into the evening. He goes to bed with a blood sugar still around 200mg/dL.
His standard deviation also gets higher throughout the day. Standard deviation on the graph is represented by the yellow and gray lines that get wider as the day goes on.
John’s low alert is set at 70 mg/dL, but it turns out his high alert was set at 250 mg/dL, so he was only being notified if his blood sugar got above 250!
He told me he set his alert so high because he didn’t want to be bothered by the alarms. Believe me I get it, but his upper alert was way way too high. I want to improve his time in range of 70-180 mg/dL, and doing so will automatically lower his time above that range. Once he hits 250 mg/dL he’s already way out of range, requiring a correction dose that may not even work well since his blood sugar is already so high.
The Solution:
I had several recommendations for John. The first was to lower his upper alert value to at least 180 mg/dL, but preferably to 150 or 160 so he could have time to act on an elevated blood sugar before it gets to 180.
My other instruction for him was to utilize his trend arrows. If he were to hit 160 with a horizontal trend arrow, for example, he may not need to act because his hybrid closed-loop system will give him little bits of insulin to bring him down to 110-120. However, if his trend arrow is going up (either diagonally up or straight up) he should consider giving himself a correction dose to bring his numbers back down into the desired range.
I also showed John how to create an alternate alert schedule for overnight so he won’t be bothered as much by alarms while he’s sleeping. His upper alert is now set to 200 when he goes to bed, but his lower alert stayed the same. During the day, he’s notified earlier by a lower high alert so he can take action.
The final change we made was to explore all the different alert sound options on his CGM so he could get rid of the annoying factory-set alarm and pick something he likes better.
The Takeaway:
Based on the one simple change of adjusting John’s upper CGM alerts, his average blood sugar will come down, his estimated A1c will come down, his standard deviation will improve, and his time in range will improve. And all without affecting his time below range. I predict his whole attitude will be completely different when he gets an alert now, and instead of saying, “Oh crap,” he’s going to say, “Awesome! I can catch this and do something about it before it gets too high!” Okay maybe not with all the exclamation points, but I guarantee he’ll be happier and better off than he was before.
Additional Resources:
How to Improve Your Time in Range Solely by Adjusting Your Alerts and Alarms!
What’s Trending in Diabetes? Trend Arrows and How to React to Them!

So how do I create an alternate alert schedule for overnight?
If you have a Dexcom, go to settings, then click on alerts, then look down and there’s a button that says alert schedule. Turn it on and it will open up options for when you want it to start, what time you want it to finish, and what you want your high and low alerts to be. You can also name it “night” if you’d like. And remember you can change the sounds if you don’t want to use the factory set ones.
Thanks. I’m trying this too!! That is me to a T!!
Let us know how it works for you!