
If you take mealtime insulin, you need to know how much to give with each meal. How do you determine your dose? The latest diabetes eating fashion is to count the carbohydrates, and use an insulin-to-carb ratio to figure out how much rapid-acting insulin to take for the meal you are about to consume (or inhale, if you are a rapid eater!)
The Insulin-to-Carb Ratio
In order to figure out your approximate insulin-to-carb ratio, take your total daily dose of fast-acting and basal insulin and divide it into 400. For example, 40 units of a total daily dose into 400 would be an insulin to carb ratio of 1:10.
A typical insulin-to-carb ratio for someone with type 1 may be 1:15 (for every 15 grams of carbohydrate consumed, 1 unit of rapid-acting insulin should be given). If someone with a ratio of 1:15 is about to eat 90 grams of carbohydrate, the dose of rapid-acting insulin for that meal would be 90/15 or 6 units. This amount would be in addition to a correction dose if the pre-meal glucose level was high or above your goal range.
The Correction Factor
To figure out your correction factor, take your total daily dose and divide it into 1800. Using a total daily dose of 40, 40 into 1800 is 45. That means one unit will drop your blood sugar 45 points. This is also called the sensitivity factor.
Someone with type 2 diabetes may have an insulin-to-carb ratio of 1:10 or even 1:5, and would take 9 or 18 units for a meal with 90g of carb.
Keep in mind, this is the typical way we calculate people’s initial doses, and it’s rare that it would be perfect for everyone, so you have to adjust by testing. By pre-meal and post-meal testing, or looking at your CGM over time after eating, you can determine your appropriate ratio. And, of course, your ratio will not work perfectly all the time, so don’t expect it to do so.
The W.A.G Approach
It’s important to note that many people with type 1, and especially type 2 diabetes, do pretty well guesstimating their dose based on past experience and trial and error. Some of us call it the W.A.G. (wild ass guess!) approach. For many of us, we are creatures of habit and eat the same amounts and types of food most of the time. I suggest using an insulin algorithm based on personal experience, trying different doses with certain types and amounts of food. In a short time, with the help of pre-meal and post-meal home glucose monitoring or CGM, most of us will have a fairly well-defined mental “insulin menu.” An insulin menu is basically how much insulin you need for a certain type of food. For example, when I eat my usual three slices of pizza, I always add an extra 8 to 10 units of my rapid-acting insulin to my usual dose to avoid excessively high post-meal glucose values (see table below).
In summary, it is important to figure out your dose of insulin at mealtime for the amount of food you are going to eat, and correct for a high blood glucose level if you have one.
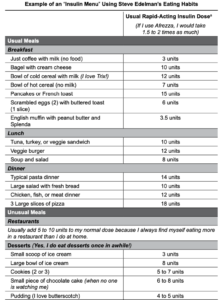
Note: These doses are my usual normal pre-meal dose of Apidra, Humalog, Novolog, Fiasp, or Lyumjev. Afrezza would be 1.5x the dose in general.
Additional Resources:

Just saw your video on glucose monitoring. Im a 67 female, high blood ptessure & last time at dr tested for pre diabetic, that eas 7 months ago. Have had hip replacement, bad knees, pain & exercise is tough. Planning on replacement in fall, but scheduled for next dr visit in 2 weeks. I know i will get strongly talked to, he kind of intimidates me, but reading all your info i think if o test higher now for type 2 diabetes, i feel like i can handle it better. Losing weight is a big thing, but again exercise is limited.. im very nervous seeing my dr.
Glad we could help – we’re going to be posting a new section in our video vault soon on exercise and losing weight so keep an eye out for that. And we have lots of great videos and articles on living well with type 2!
explain how you dose for icecream and pizza with Fiasp. I’m experimenting with 50/50 and should have taken the 50% 2 hours and not 3 hours after eating… we’ll see:) I’m T1 with CR 18
I think you said the magic word: experiment. It’s trial and error. Your approach sounds good, however there are many variables…what kind and how much ice cream, how much pizza, was there any activity before or after eating, etc. When you experiment, try to be consistent.
Hi Guys,
I’m a type 2 for many years, controlled with oral meds. My Endo recently added Humalog to help with my after meal spikes. Can you give me some hints on dosing? Max dose? Before or after meals? Every meal? Any ideas would be greatly appreciated!
Hi Warren,
Everyone is different, but if you haven’t yet seen Gary Scheiner’s article on controlling post-meal spikes, I highly recommend it:
https://tcoyd.org/2019/10/strike-the-spike-controlling-blood-sugars-after-eating/
Hope that helps!
Thanks for the info!
“ In order to figure out your approximate insulin-to-carb ratio, take your total daily dose of fast-acting and basal insulin and divide it into 400.”
How does one figure out one’s “total daily dose” in the first place?
Get out your abacus and add up your basal and your fast-acting insulin…in general how much you take every day. That formula is just a basic place to start. It may not be perfect, but it should be in the ballpark.
Looking over many diabetic articles and info.Have type2 and diabetic family members type 1 and 2.This has been the most informative site.In simple terms.Thank you.its been continually helpful.
Glad to hear that. Let us know if you have any questions!
New to this still not sure had to long active
I have cut out sugar and starch. I struggle to get my levels mostly between 9 and 11. I use mostly oats flour and Stevie sweetener. Main meal is mostly chicken and vegs
Hi Louisa-Jane,
It sounds like you may need an adjustment in your therapy. Since I don’t know the medications you’re on, I really can’t make any suggestions. However, whatever you’re taking it sounds like you need more of it, or an additional diabetes drug or injection, so best to speak with your caregiver.